Pet Oral Surgery for Complex Oral Conditions
Dental care plays a vital role in your pet’s life and most cats and dogs at some time may need oral surgery treatment to keep them healthy and pain-free. Our veterinary dentists have extensive training in oral surgery, anesthesia, pain management, diagnosing and treating various oral conditions. Therefore, we are well-equipped to address your pet’s problem and help you find a solution.
For general practice veterinarians, pet dental surgery is limited to basic tooth extractions and the occasional oral tumor removal. At Dallas Veterinary Dentistry & Oral Surgery, our dentists are trained to provide treatment for difficult cases, allowing your precious family members a better quality of life. Call us today at (817) 431-8451.
Surgical Procedures
Our specialists have broad experience performing complex oral surgeries, such as:
- Difficult tooth extractions (and full-mouth extractions)
- Jaw fracture repair
- Palatal defect correction (cleft palate, elongated soft palate)
- Oral tumor removal
- Oronasal fistula repair
- Treating dislocated teeth
- Oral trauma repair
When Are Tooth Extractions Necessary?
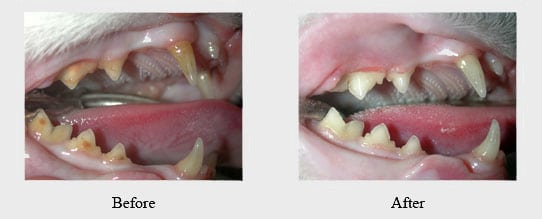
Extraction is often the ideal treatment for feline tooth resorption and feline gingivostomatitis. However, it may also be necessary for chipped, fractured, and/or diseased teeth that cannot be saved. In such cases, the best way to ensure pain relief and improved oral health for your pet is to remove those teeth. With extractions, our specialists take full-mouth radiographs to evaluate the damage before surgery and to check for remaining tooth roots after surgery.

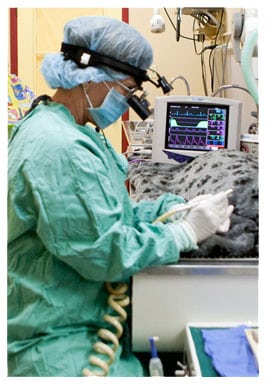
Reducing Pain and Safety Risks in Surgery
As fellow pet owners and animal lovers, we understand your concerns about general anesthesia and pain management. Your pet will receive customized care that considers their age, size, breed, health, and current oral condition to keep them as safe and comfortable as possible. We carefully measure and administer anesthetic and pain relief medications with your pet’s needs in mind. Additionally, we always suture extraction sites to prevent dry socket. This painful condition occurs if the blood clot that forms following tooth removal dissolves or gets dislodged.
Our Capabilities
Our specialists received comprehensive training in animal anesthesia and pain management and are both Diplomates of the American Veterinary Dental College. This is the most advanced training that can be achieved in veterinary dentistry. Furthermore, our facilities offer innovative technology that gives us an advantage in identifying, diagnosing, and treating complicated dental issues. We far exceed the American Animal Hospital Association's guidelines to provide advanced pet dental surgery in a safe, welcoming environment.